Departments
Esthetics
Sep 2007 —
Vol. 1,
Iss. 1
Changing Tooth Position With Orthodontics or Restorative Dentistry: Both Perspectives
Dentistry often provides multiple treatment options
for patients. The treatment planning
process is difficult because various options
present advantages and disadvantages for individual patients and, therefore, must be
customized for each case. Tooth replacement is
a common example, as it can be accomplished with removable partial dentures, fixed bridges, or implants. The
appropriate treatment is based on
constraints such as financial limitations, patient preferences, long-term prognosis, patient comfort, physical
barriers, psychological considerations, and the
dentist’s and laboratory’s ability
to perform the work. Treatment planning to correct misaligned teeth is
similar.
Correcting the appearance of misaligned teeth is
accomplished with
orthodontics, restorative dentistry, or both. Tooth misalignment includes tooth rotation, crowding, super-eruption,
under-eruption, intrusion, diastemas, and
labial, lingual, mesial, or distal tipping.
Misalignment also occurs from
inappropriate arch shape, position and size, and arch-to-arch relationships. Correction with
orthodontics or restorative dentistry presents
limitations, advantages, and disadvantages.
Restorative Techniques and Limitations
It is important to understand what can be achieved
with restorative dentistry, orthodontics, and
combined treatments. Restorative dentistry
changes tooth morphology by removing tooth structure or adding restorative materials to
replace missing tooth structure and increase
dimensions. Changes are made to the coronal portion
of a tooth without movement of the root. The root dimensions at the cemento-enamel junction or where a root exits the
gums and alveolus cannot be moved restoratively and, therefore, become
a limiting factor. Orthodontics is required to change root position. Consequently, maximum and minimum tooth width is determined by the root position
of a tooth and the adjacent teeth.
Tooth reduction is a second limiting factor. Removal
of tooth structure must leave sufficient support
to resist forces without fracturing. For
example, a lateral incisor that has a small cross section following crown preparation can fracture through
dimension, leaving the coronal
portion of a tooth in a crown. Reduction cannot encroach on the pulp or it will lead to pulpal necrosis
unless endodontic treatment is planned.1-5 Removal of enamel
that exposes dentin must allow enough room to
restore over dentin to prevent sensitivity.2,6-8
Restorative Illusions
Changes in tooth anatomy without altering overall
tooth dimensions can create an appearance
of tooth movement. Controlling the face
and silhouette of a tooth provides visual indicators of perceived size and
long axis orientation. A large tooth looks smaller
when the face is small, while the silhouette fills the space, thereby not requiring a change in existing tooth-to-tooth space.9-12
The face of a tooth is defined as the central portion
of a facial surface within the mesial and
distal line angles, the gingival height of contour and the incisal edge or transitional incisal
curvature.9-12 The silhouette is defined by the
outside edges of the tooth, including
the gingival contour, gingival and incisal embrasures, contacts, and incisal edge.9-12
The face of a tooth looks smaller as line angles,
gingival height of contour, and incisal
curvature approach the center of a tooth.9-12 Curved line angles, combined
with increased embrasure size, reduce the
incisal length to create a smaller appearance. Color variation, as well as surface contour and
texture of the face of a tooth, make teeth look
smaller, wider, or longer.9-12 For example, 2 vertical
grooves between lobes of a central incisor create a longer looking tooth,
while horizontal grooves make a central incisor look
wider. Ideally, placement of grooves or surface texture should replicate naturally occurring patterns.
Case 1
An incisal fracture and chipping on the left central
incisor require restoration to recreate
proper anatomy (Figure 1 View Figure). Further evaluation reveals rotation of the
tooth (Figure 2 View Figure). Composite is added to the facial surface and
restores the incisal edge. Increased thickness
at the incisal edge from increasing the facial dimension creates a more durable restoration and reduces the
appearance of misalignment/rotation (Figure 3 View Figure).
This tooth could have been rotated orthodontically, but doing so would not
have rendered a superior esthetic result (Figure 4 View Figure) and would have compromised the durability of the
final restoration by under-utilizing the bonding surface on the facial aspect.
Restorative Treatment Planning
Improving smiles takes into consideration 3 major
defect categories: tooth
position, color, and loss of tooth structure. Changing the appearance of tooth position with restorative dentistry
may be preferable
to orthodontics if restoration is required to correct color flaws or loss of tooth
structure.13 Tooth color defects include discoloration, stains, fluorosis, tetracycline
stains, decalcifications, hypocalcifications,
craze lines, fillings, root exposure, and cavities. Tooth structure
losses include chips, cracks,
abrasion, attrition, surface defects,
exposed root structure, surface contour defects,
surface texture defects, factures, cavities,
and developmental defects such as
amelogenesis or dentinogenesis imperfecta.
When treatment planning, existing tooth position is compared to ideal tooth position. Tooth
structure outside the ideal position requires
tooth reduction. If the magnitude of reduction extends beyond
enamel into sensitive dentin, extra reduction is required so that a restoration can cover the dentin
surface. Teeth require restoration to add tooth mass if
the ideal tooth position is outside of the existing position.14,15 Drawing teeth 2-dimensionally from an occlusal or facial
perspective can help develop the restorative
approach. The technique of drawing is
effective for very experienced dentists who can
envision objects 3-dimensionally from a
series of 2-dimensional images.
Diagnostic wax-ups create 3-dimensional images and
predictable results. Wax is added to areas that require increased
dimension, and the diagnostic models are marked to indicate areas of reduction. Alternatively, a duplicate model can be
trimmed extensively, and the teeth can be
waxed to full contour. A visual comparison is made of the original study
model and the ideal waxed model. An impression of a waxed model is poured
in stone, and a clear vacuum form is used as a
template to verify treatment progress
intraorally.
Case 2
In this unaesthetic smile (Figure 5 View Figure), the teeth have
dark and irregular
color patterns. Wear has reduced incisor length, chipped teeth unevenly and developed irregular facial contours. Loss of
posterior support has caused the maxillary
cuspids to flair buccally (Figures 6 View Figure and 7 View Figure).
There are minor irregularities in the gingival
contours, especially around the right central incisor.
A drawing of the existing tooth shape and position in
red, with an ideal tooth position and shape in blue, was rendered (Figure 8 View Figure). Areas where blue lines are outside of red lines
required the addition of tooth structure or
gingival recontouring, while areas
defined by red lines outside of blue lines required
reduction. Three dimensionally, the
cuspids required extra preparation to reduce the
buccal flair, while the lingual tipped incisors required less reduction and additional material to produce a
more buccal position.
In this case, the patient’s teeth required
restoration for defects in tooth color and structure (Figure 9 View Figure), and it was determined
that correction of
the appearance of tooth position could be accomplished at the same time. Evaluation
of the primary 2 limiting factors of
restorative treatment alone (i.e., root position and the amount of remaining tooth structure) revealed that orthodontics was not required to supplement treatment. Full-mouth reconstruction without
braces resulted in a perfect smile (Figure
10 View Figure).
The Orthodontic Perspective
The ability to physically move teeth presents myriad
possibilities that
could substantially improve many patients’ appearances. When an orthodontist evaluates a
case for treatment, he/she is considering
a variety of functional and esthetic goals. First and foremost, an orthodontist looks at the basic functional guidelines
learned in dental school: overjet (i.e., how
much the top teeth flare labially from the
bottom teeth); overbite (i.e., how much vertical
overlap exists between the front teeth); transverse relationship between upper and lower teeth; facial profile;
crowding/spacing; excursive movements; etc. It is oftentimes an
aberration in these basic guidelines that prompts a referral to an
orthodontist. These are well understood principals; but what about the
more subtle concepts? What can an orthodontist do for patients who have some restorative needs or are simply displeased with
the esthetic appearance of their
smiles?
The first thing all orthodontists should do in an
examination is look
at a patient’s smile. It sounds obvious, but it is rarely done. Patients should smile naturally and laugh so they can
be viewed very critically. Does the patient show
any gingiva? Are the patient’s
gingival margins esthetic? Is the patient’s maxillary dental midline
coincident with their facial midline? Do the patient’s maxillary incisal edges follow the contour of their lower lip?
Are there black
spaces in between the contact points of adjacent teeth and the papilla? Do the teeth look symmetric and proportional
vertically and horizontally? Are the patient’s buccal corridors
filled with nicely colored tooth structure or
black cavernous spaces? Are there large spaces, areas of crowding, tipped teeth, or unevenly worn teeth? These are all common findings that an
orthodontist has the ability to
manipulate.
If a patient shows gingival tissue when smiling, it is equally important to treatment plan gingival esthetic goals because it is a dental esthetic goal. Zero to
2.0 millimeters of gingival display is highly esthetic and appears youthful.16,17 As a general rule, a
patient’s gingiva should appear 0.5 mm to 1 mm higher on the central incisors and canines
than the lateral incisors.18 Most importantly, however, similar classes of teeth should appear symmetric bilaterally.19 Gingival margins that do not follow this general guideline appear uneven, thereby making some teeth appear too
high/low or disproportionately long/short. In
the absence of periodontal disease or any other
complicating factors, the gingival margins will follow teeth as they are moved and afford an orthodontist the opportunity to
manipulate their positions as they
reposition teeth.20
Of the many complicating factors impacting an
orthodontist’s ability to achieve
perfectly esthetic gingival margins are
variations in tooth proportions. This is a very common problem among adult
patients because misaligned teeth are usually worn unevenly. When this is
the case, an orthodontist, working in conjunction with a restorative
dentist, should evaluate tooth proportions to determine whether the longer
adjacent teeth should be recontoured at their incisal edge to match the
worn tooth, or the worn tooth built up to match the longer, unworn
contralateral tooth. That determination is commonly based on the rule of golden proportions that outlines the appropriate sizes of adjacent teeth in an arch.21-24
Using a central incisor as a frame of reference, we
know that the ideal width-to-height ratio in most faces is between 75% to
80%.25,26
If, for example, a central incisor is 8.75 mm wide, its height should be between 11.7 mm for a longer appearing tooth and 10.9 mm for a shorter
appearing tooth. If the gingival margin of this 8.75-mm wide tooth is at 1.5 mm incisal to the ideal
gingival margin position, and the unworn adjacent tooth is sized
according to the dimensions above, we would intrude this tooth to achieve esthetic gingival margins and build up its height to the properly sized adjacent
central incisor. If, on the other hand, the adjacent unworn central incisor
was more than 12.4 mm (e.g., 10.9 mm plus 1.5
mm), we would extrude the unworn central incisor
to achieve esthetic gingival margins and enamelplasty its incisal edge so that it matches the proportions of the worn,
but proportionately sized, adjacent central
incisor. Naturally, some situations warrant a combination of both
approaches.
Once the ideal gingival margin locations and tooth
proportions have
been identified, teeth can be positioned to distribute spaces ideally for restorations.
Ideally positioned tooth preparations will allow
for more uniform tooth reduction and restoration; decreased areas of heavy reduction and
subsequent pulp exposures with future
maintenance restorations; decreased periodontal complications from overbulked restorations; and highly esthetic emergence profiles.27 If, for example, space is needed for restoration of a
pegged lateral incisor, it should be positioned so that two-thirds of the space is distributed on the distal side of the
tooth and one-third of the space is distributed
on the mesial side.27 If this same tooth is positioned
with the majority of the space on the mesial,
this side will be overbulked and generate an overly acute emergence
profile. Remember the rule about gingival margin levels? It is also
imperative that pegged laterals be positioned vertically to generate a
gingival margin that is symmetric with the contralateral incisor gingival
margin.
Unfortunately, even the best sized and proportioned
teeth can still look awkward if the midline of the maxillary teeth does not align with the middle of a patient’s face.
Treatment of a non-coincident midline greater than 1 mm
would involve physically moving teeth
orthodontically. Very large movements may even
involve the reduction of tooth mass using interproximal reduction or
asymmetric extractions.
Additionally, well-aligned teeth do not look natural
if their incisal edges do not follow the contour of a patient’s lower
lip. Maxillary arches that appear linear transversely look very artificial.
The vertical dimensions of the maxillary incisors, however, cannot be
augmented too much before they stand in violation of generally accepted
esthetic tooth proportions and appear very long and slender.21-26 That is, of
course, unless that patient has inadequate incisal display when they smile
and hides the excess crown length behind their
upper lip. It is imperative, therefore, that
orthodontists position teeth in a way that is vertically harmonious with
the shape of a patient’s lower lip when they smile.
A maxillary arch that follows the mandibular lip
contour should also diminish into a
patient’s cheeks and not appear to end
abruptly distal to the patient’s canines.28 This objective is loosely referred to as a broad smile or narrow smile,
but more precisely described
by a qualification of buccal corridor volume. Treatment of a patient with large
buccal corridors has to proceed cautiously,
because expanding the transverse dimension of the maxillary arch so that it is disproportional with the mandibular arch
would introduce a significant
functional compromise. Additionally, this movement
in a patient with a resistance at the mid-palatine suture would merely tip teeth buccally and, consequently, be unstable and potentially detrimental to long-term gingival health (recession).29
Conclusion
Changing tooth position may involve and take into
consideration orthodontics and/or
restorative options. Thorough diagnosis of tooth position, structure, and
color are required for treatment planning. Patient goals and limitations to
treatment define expected results, as well as the most appropriate
option selected.
References
1. King M. Preserving the vital pulp in
operative dentistry. ent Update. 2003;30(3):159.
2. Tecles O, Laurent P, Zygouritsas S, et
al. Activation of human dental pulp progenitor/stem cells in response to
odontoblast injury. Arch Oral Biol. 2005;50(2):103-8.
3. Vij R, Coll JA, Shelton P, et al.
Caries control and other variables associated with success of primary
molar vital pulp therapy. Pediatr Dent. 2004;26(3):214-20.
4. Bichacho N, Eylat Y, Dadi M, et al.
Restoration modalities of severely injured anterior teeth gingival
integration, papillae support, and predictable imperfections. Compend
Contin Educ Dent. 2003;24(12):891-4, 896-8, 900-4.
5. Scarano A,
Manzon L, DiGiorgio R, et al. Direct capping with four different materials
in humans: histological analysis of odontoblast activity. J Endod. 2003;29(11):
729-34.
6. Magne P.
Immediate dentin sealing: a fundamental procedure for indirect bonded
restorations. J Esthet Restor Dent. 2005;17(3):144-54.
7. Bassi GS, Youngson CC. An in vitro
study of dentin exposure during resin-bonded
fixed partial denture preparation. Quintessence Int. 2004;35(7):541-8.
8. Lockard MW. A retrospective study of
pulpal response in vital adult teeth prepared for complete coverage
restorations at ultrahigh speed using only air coolant. J Prosthet
Dent. 2002;88(5):473-8
9. Chalifoux
PR. Checklist to aesthetic dentistry. Pract Periodontics Aesthet Dent. 1990;2(1):9-12.
10. Singer BA.
Principles of esthetics. Curr Opin Cosmet Dent. 1994;6-12.
11. Singer BA.
Fundamentals of esthetics. In: Dale BG, Aschheim KW, eds. Esthetic Dentistry: A
Clinical Approach to Techniques and Materials. 1st ed. Philadelphia: Lea & Febiger; 1993:5-13.
12. Chalifoux PR. Perception aesthetics
and light-cured composites. Pract Periodontics Aesthet Dent. 1992;4(5):
51-56.
13. Chalifoux PR. Perception esthetics:
factors that affect smile design. J Esthet Dent. 1996;8(4):189-92.
14. Magne P, Belser UC. Novel porcelain
laminate preparation approach driven by a
diagnostic mock-up. J Esthet Restor Dent. 2004;16(1):7-16.
15. Morgan DW, Comella MC, Staffanou RS. A
diagnostic wax-up technique. J Prosthet Dent. 1975;33(2):169-77.
16. Chiche GJ, Pinault A. Esthetics of
Anterior Fixed Prosthodontics. Chicago: Quintessence Pub.
Co.;1994.
17. Kokich VO
Jr, Kiyak HA, Shapiro PA. Comparing the perception of dentists and lay
people to altered dental esthetics. J Esthet Dent. 1999;11(6):311-24.
18. Rufenacht C. Structural esthetic
rules. In: Rufenacht CR, ed. Fundamentals
of Esthetics. Chicago: Quintessence Pub. Co.; 1990:67-135.
19. Kokich VG, Spear FM. Guidelines for
managing the orthodontic-restorative patient. Semin Orthod. 1997;3(1):
3-20.
20. Kokich VG, Kokich VO.
Interrelationship of orthodontics with periodontics
and restorative dentistry. In: Nanda R, ed. Biomechanics and Esthetic Strategies in Clinical Orthodontics. St. Louis:
Elsevier Saunders; 2005:
348-373.
21. Lombardi RE. The principles of visual
perception and their clinical application to denture esthetics. J Prosthet
Dent. 1973;29(4):358-82.
22. Levin E. Dental esthetics and the
golden proportions. J Prosthet Dent. 1978; 40:244-252.
23. Brisman AS. Esthetics: a comparison of
dentists’ and patients’ concepts. J Am Dent Assoc. 1980;100(3):
345-352.
24. Qualtrough AJ, Burke FJ. A look at
dental esthetics. Quintessence Int. 1994;25(1):7-14.
25. Gürel G. The Science and Art of
Porcelain Laminate Veneers. London, Chicago: Quintessence; 2003.
26. Gillen RJ, Schwartz RS, Hilton TJ, et
al. An analysis of selected normative tooth proportions. Int J Prosthodont. 1994;7(5):
410-7.
27. Kokich VG. Managing
orthodontic-restorative treatment for the adolescent patient. In: McNamara
JA Jr, Brudon WL, Kokich VG, eds. Orthodontics and Dentofacial
Orthopedics. Ann Arbor: Needham Press, Inc.; 2001:395-422.
28. Sarver DM. Principles of cosmetic
dentistry in orthodontics: Part 1. Shape and proportionality of anterior
teeth. Am J Orthod Dentofacial Orthop. 2004;126(6):749-53.
29. Carmen M,
Marcella P, Guiseppe C, et al. Periodontal evaluation in patients undergoing
maxillary expansion. J Craniofac Surg. 2000;11(5):491-4.
Note: All photographs are published with permission from www.dentalcomposites.com.
 |
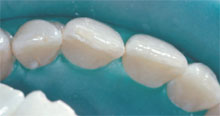 |
| Figure 1 Preoperative view of a patient with an incisal fracture. |
Figure 2 Further evaluation reveals tooth rotation. |
| |
|
 |
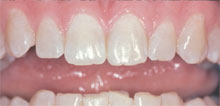 |
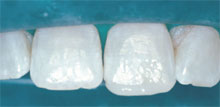
| Figure 3 View of the composite build-up prior to surface contouring
and texturing, incisal edge characterization, and polishing. |
Figure 4 The final restoration demonstrating how tooth anatomy,
color, and position blend with the surrounding teeth. |
| |
|
 |
 |
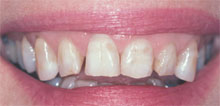
| Figure 5 Preoperative view of a patient with excessive wear,
chipped teeth, and irregular facial contours. |
Figure 6 View demonstrating how loss of posterior support has
caused the maxillary right cuspid to flare buccally. |
| |
|
 |
 |
| Figure 7 Alternate view demonstrating the same effect on the
maxillary left cuspid. |
Figure 8 A 2-dimensional drawing of the existing tooth shape and
position in red, with the ideal position and shape in blue, to determine
areas requiring reduction and addition of mass. |
| |
|
 |
 |
| Figure 9 Preoperative full-facial
view. |
Figure 10 Postoperative fullfacial
view. Evaluation of two primary
limiting factors of restorative
treatment alone revealed that
orthodontics was not required
to achieve this exceptionally
esthetic result. |













